|
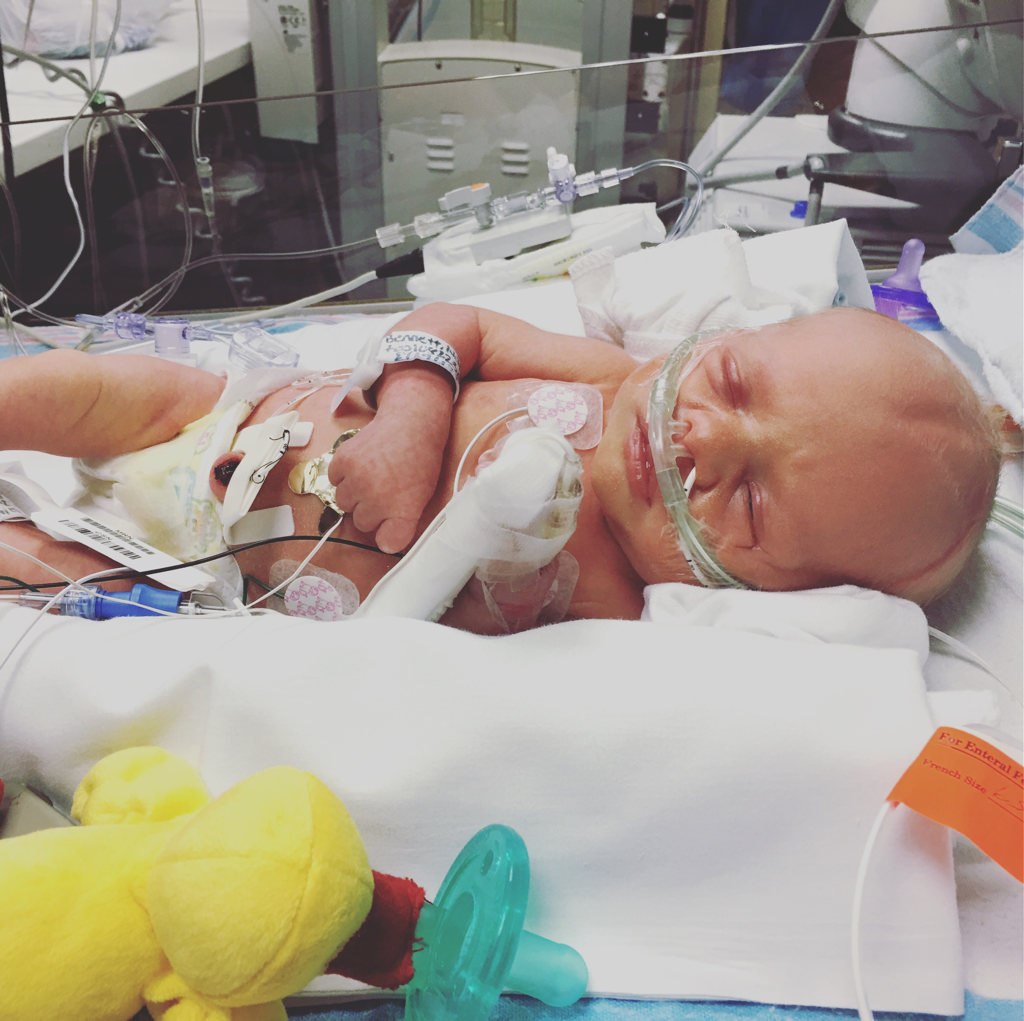
After Birdie was born, she was transferred to the neonatal intensive care unit or NICU to immediately address her respiratory distress. Along with her immature lungs, she was thought to have aspirated some fluid during her abrupt entrance in to this world. There were some complications during my c section that resulted in Squeak being yanked a few times from my rib cage. She required breathing assistance via a CPAP for about 24 hours before she was weaned off oxygen for another 3 days.
After my blood pressure stabilzed, my hospital bed was wheeled to the NICU and I was allowed to see my tiny miracle for about 5 minutes before being taken to the postpartum unit. Again I was without my baby in my arms, but she was alive. They told me to sleep. Yeah. I stared at the clock willing the feeling to return to my legs so I could crawl to my child. I called the NICU every 45 minutes to ask about our baby. The anguish of our first child dying and then watching Birdie struggling to breathe was enough to crack the strongest of people. This experience has easily shaved 10 years off my life and there will never be enough concealer to rectify the bags under my eyes. When Birdie started experiencing apnea episodes and I watched all of her numbers plummet and our girl essentially hold her breathe, I do not have the right words. It's a special level of fear hearing alarms go off and everyone rush to your child's bedside. I wanted it to be me. I begged for it to be me. It's watching your heart beat outside your body and you can do nothing to control what is happening. Fortunately the staff realized very quickly what this issue was and the appropriate medication administered. The medication thankfully resolved the apnea of prematurity issues immediately but I'll watch her breathe until she's 18.Then we tackled the bottle feedings. Preemies have difficulties coordinating the whole suck-swallow-breathe situation, while eating. My kid didn't even get a go at a bottle for 8 days due to oxygen needs. Thanks to a mighty NICU speech therapist, my kid can now eat. Eat a lot. At 4 am. Fun side note. I AM a pediatric speech therapist and MY kid ate better for the NICU speech therapist, Beau and pretty much any nurse. I sobbed in my car on more than one occasion. Thats what the NICU feels like. Holding your breathe. Waiting for the bad, waiting for the good, waiting. Tip toeing through the day. Counting every mL drank and the scale move up by grams. I've googled how many grams to an ounce, ounce to lbs more than I care to admit. The NICU is driving away from the hospital, trusting other people (very awesome,capable people) to watch your baby so you can have a break from the hospital room. The NICU is walking past the well baby nursery, top full of crying, fat babies and grieving your birth plan. My birth plan did not involve my guts being removed. I've had one baby vaginally and one via c-section. Folks, c-sections are not the easy way out. I'll post about that on a later date. It's fighting the guilt. You should feel nothing but happy and gratitude for your tiny baby but you can't help but cry. The baby blues are a real thing. I cried over everything. We are on high alert for any post partum anxiety or depression as parents who have experienced child loss are at higher than average risk. I am pretty in tune with my feelings but I still have a counselor and my family keeps an eye on things. My hormones are a little more even now but I just cried because she's another day older so there's that. The NICU is hard on your marriage. While Beau had all the faith in the world about our medical team I felt the need to be there every second I could. I would get really snippy about having to leave and I'll give you a guess who had to deal with my madness. I'm sure I set a record for the number of questions I asked or things I worried about. But I'll continue to stand on my soap box about how love conquers all and marriages should evolve, bend to withstand life. I made a grand life choice in making Beau my partner, he is for sure the calm to my storm. Love you babe. The phenomenal NICU nurses, Beau, families and our well established tribe helped me keep in together as best as possible. Reaching out to a friend who had two babies in the NICU was a vital life line. Having someone tell you it's ok to cry for 12 hours for no reason or for a reason helped me to feel validated. If you ever know someone or are someone experiencing a NICU stay I'd be happy to talk to you and have a party over every mIlliliter your kid drinks. Every day that monitor doesn't sound. Cry with you. Bring you a beer. Im grateful our NICU stay was 21 days. I know many a brave families experiencing longer stays or parents of babies with critical issues. I'll tuck you right in my heart with my girls. Rest easy Pipes.
1 Comment
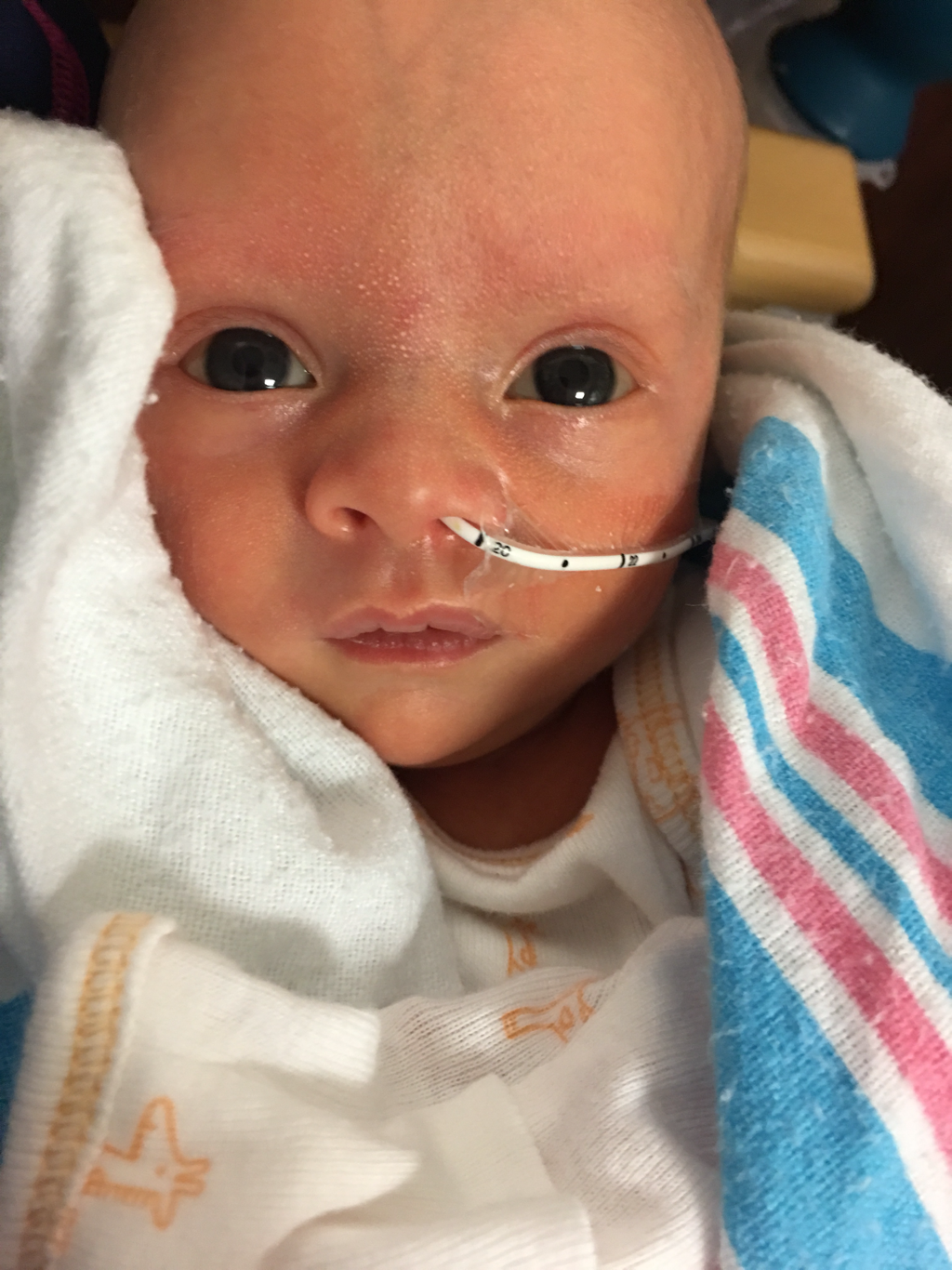
My tiny miracle, our rainbow of hope made a dramatic entrance via emergency C-section, August 19th at 8:55 p.m., at 35 weeks and 1 day. Weighing 4 lbs, 9 ounces and 17.25 inches. She immediately opened her eyes and Squeaked.
Our birth story is a scary story with a very happy ending. Let me tell you how kick counting saved my baby. Early that same day I noted baby bird was moving less frequently. After monitoring her movements for an hour I was overcome by fear and an extreme urge to go to L&D. Call it mothers instinct. I had counted kicks several times a day since week 28 per our doctors suggestion. If you are not familiar with kick counting, it's when you pick 1-2x a day, when your baby is most active, to monitor their movements. You should ideally feel 10 movements in an hour. I used an app on my phone or a post it on my desk. Birdie, like her sister, was very active in utero and rarely made me "worry" about lack of movement. Typically following cold water and a lay on the couch, I would get 10 movements under 10 minutes, but never longer then 30. I felt 3 in 45 minutes. My mom drove me as Beau was out of town for the day. It was the longest drive of my life. Upon arrival to the hospital, I began to hyperventilate and experience the worst panic attack of my life, fearing the absolutely worst. I was in respiratory distress by the time I made it to L&D and immediately hooked up to a fetal doppler, revealing a slow but present heartbeat. Initially they said she was "sleeping" but I knew my baby and knew that heart rate was far too low following the dozen or so NSTs. I adamantly said over and over, very loudly, that something was wrong. Fortunately, my concerns were not ignored and my doctor was paged. Slowly the heart rate began to decline. I was flipped on my side and pumped full of juice in an effort to wake baby. I required oxygen as I continued to hyperventilate. "Deep breathes" the nurse chanted. An IV line was started and baby did begin to show some small accelerations. I can not even begin to explain the fear. Two of Piper's nurses were there and took turns sitting with me on my bed as my mom tried to keep Beau up to date. Doctor arrived and started a biophysical profile. After baby did not move for several minutes she exited the room and returned very quickly. "Ready to have baby, today?" She had confirmed with our speciality team that baby was in distress and was better out out than in. As I briefly panicked about having a preemie, my doctor said we have everything to lose by leaving her in my belly. Things moved fast from that point as I was prepped for surgery. Beau was racing down down the interstate to be by my side as I sat in the brightly lit operating room and my spinal tap was put in. I'd like to say I was handling this with grace but in reality after I was numb, I began thrashing around in panic. I couldn't feel anything from chest down and while that's the game plan the loss of what little control I had went out the window. I began screaming and needed to be strapped down. And later medicated. The amazing surgical team kept telling me this was to save our daughter. My mom sat with me as Birdie was delivered, with a yank and a squeak. Beau entered the room as they lifted her above the screen. She was breathing on her own and had a heartbeat, not needing resuscitation, but needed a few minutes to fully come around. "Happy Birthday", said our doctor. Silence. "There's a true knot in her cord". You can read that line as many times as I've replayed it in my head. The anomaly we had been assured would not reoccur, almost claimed our second daughter's life. We have been told in is a 1 in 10,000 occurrence, and we should be things of medical textbooks. Lightning struck twice, but this time I was ready. With all the testing we had done, kick counting and motherly instinct is what saved my daughter. Theory is when she flipped back breech she pulled her cord too tightly, similar to Piper except that she pulled hers engaging for birth. It's also their thought that it was tight enough to restrict growth but not tight enough to register on any of their tests. We are hoping to have more answers at our 6 weeks follow up with the specialist. The rarity of this may have an underlying genetic component. She had consistently measured in the 2nd percentile but was born closer to the 13th with her head in the 75th, gestationally our neonatologist believes she was closer to 34 than 35 weeks. Without Gods grace, our daughter would have lived only another hour or two. I can't focus on the fact too long or I won't make it. The responsibility is too heavy and the what ifs too much to handle. Birdie is HOME following a 21 day NICU stay, secondary to prematurity. She is a born fighter. She's now 5 lbs 2 ounces,18 inches of pure JOY. She is everything and more that I've dreamed about for 8+ months, for my whole life. While it will never be fair or make sense as to why we don't have our two blondes together, in this life. Piper sent Birdie to us and gave me the knowledge to save her sister's life. Rest easy Piper Kai Bennett, we miss you everyday. I've started this entry so many times. It's difficult to organize my thoughts. My journal entries are messy. The are full of incohesive lists, thoughts, bargains with the universe and in the most recent ones loads of swearing. The indentifiable downfall following Pipers day, coupled with third trimester anxiety made a perfect storm for a deep state of sadness. I've been akin to an obese sloth, moving as little and slowly as possible. I went in to my biweekly appointment a few weeks ago, on an upswing and eager to sneak a peek at my tiniest nugget. Fluid levels all fine so off to our NST. We got high marks on our heat rate test and as I'm feeling smug, the doctor came in with my ultrasound in hand. Moms out there, you get that feeling things are about to go down? Doc says, they found something ""concerning" and wanted me to follow up with our specialty team that Monday. We were already heading in to see our MFM specialist Monday to check growth. He says "don't worry". Yeaaah. I hate to be vague especially when we are so open about our PAL journey but I can't even go in to the details without shaking. I googled myself right on in to a panic attack. Not a figure of speech, an actual panic attack, with respiratory distress and all, where I could not drive my car out of the office parking lot. Mama Bear Bowen has since nixed anymore appointments without an escort. I spent three days crying on my couch. Driving Beau within an inch of what little sanity he has left. My anxiety finally got the best of me Saturday evening. I felt that Squeak hadn't been moving enough so I had my Beau drive me to L&D. He drove fast. Neither of us had been on that floor in the hospital since we had left without our big girl over a year ago but my concern for Squeak was in the forefront. A potentially crippling move became a mission. One of Pipe's nurses was working, immediately recognized us and ushered us back to a room. Once the monitor was on the little bugger kicked up a storm and her tiny heart beat registered strong. All was well. The nursing staff was so very kind, reassuring us coming in is always the right thing to do. Expectant moms, trust your gut, go in immediately. You will not be that patient or an inconvenience to anyone. You are your only advocate for your baby. Babies move differently but movements do not slow down. The level 2 ultrasound on Monday, could not even locate this "concern". It was a complete non issue. What I should type here is my sense of relief but the emotion that I defaulted to, was sheer anger. I want to blame someone for the recent onset of anxiety, but all everyone is doing is looking extra close at our baby for safe keeping. So I'll settle on down as relieved and happy she continues to thrive. If you've been following our story, Squeak has kept us on our toes via several ultrasounds. The remainder of the hour long ultrasound revealed a healthy baby. All blood flow dopplers, within normal. If you have never had a blood flow doppler you should investigate this modern miracle in which they check the blood flow between me and Squeaks various organs. This is particularly comforting to me as Pipes cord was the issue. Big doc in charge comes in to chat. Squeak looks good but continues to measure on the lowest end of their growth chart. Now mind you, our second kid has been small this entire pregnancy, but took a little dip this past month. The doctors prescribed modified bed rest. The theory is more immobile I can stay, the more blood flow and good nutrients get to our girl. The less hard my body has to work for every day things like work and exercise the more energy can be spent growing her. I'm allowed up for short periods of time. I need to be sitting and ideally laying a majority of the day. I can hear you through my computer. Wow, I wish someone told me to lay about, eat all the things (ok high protein, ick), relax and get more then your fill of reality TV. Sounds nice in theory but a solid recipe for cabin fever. I am hoping it will help alleviate some of the stress this trimester has introduced. It was certainly a turn of events. Squeak and I will be here on the couch completely our mission: grow a fat baby for two more weeks then we will make some more decisions about her arrival. I have emotional whiplash but intend to be the best couch potato, ever. Rest easy PKB. |
Archives
October 2019
Categories |





 RSS Feed
RSS Feed